Intermittent Fasting for Cholesterol, Weight, Tummy Trouble & Pain
- Havilah Brodhead, RN, MSN, FNP

- Feb 23, 2021
- 13 min read
Intermittent fasting (IF) is a more than just a buzz word--it works! There is great scientific data to back it up, and the physiology of how it works makes sense. We were never meant to have 24/7 access to food, especially highly processed foods. Our pancreas, intestines, liver, and kidneys have to work overtime to compensate for that frequent feeding. Our body was meant to have breaks (fasts) from food where it can recalibrate, process, rest, and pull calories from fat stores. When we fail to give it the opportunity to do so, excess weight, glucose intolerance, and inflammation (often along with pain or belly problems), sets in. Fasting is one of the healthiest and most natural methods I've come across for overall health.
Honestly, I didn't know a lot about it a few years ago--it wasn't "taught in school". My husband had gained some extra weight after we had kids, which he referred to has his "baby weight and dad bod." He wanted to get back to a weight that felt good and allowed him to mountain bike and climb again. He dove into research on IF and then began implementing it, mixing IF with extended fasting to achieve interval weight loss and maintain weight. I soon started doing the same--a few days a week, mostly work days, which has worked well for me.
I have been able to help patients bring cholesterol levels and blood sugar levels and weights down to healthier levels combining exercise, IF, and a lower, complex carb/healthy fat/lean protein diet.

WHAT IS Intermittent Fasting and how do you do it?
Simply put, intermittent fasting (IF) is eating only during certain hours and "fasting" during others. The most popular method is to fast for 16 hours, leaving an 8 hour window when one can eat smart, balanced foods. IF has been used for decades in other countries to help with a myriad of health conditions, ranging from diabetes to joint disease, autoimmune disease and mental health. IF has been gaining a lot of scientific traction and acceptance in Western medicine here in the States over the last decade.
“Intermittent fasting (IF) dates back to the beginning of humankind when no matter how hungry, humans had to be sharp, strong and energized to find, forage or hunt for that next meal,” reports author Lucy Danzier. “Cycling through feast and famine was as natural as cycling through sleep….if all of this sounds barbaric, consider that doctors use intermittent fasting to maintain their weight and energy levels during long, grueling hours of rounds when they need to be alert.”
It’s true. My husband and I are both nurse practitioners who incorporate IF into our daily work lives to maintain healthy weights.
My husband was the one who introduced me to IF. He had gained 20 lbs after we had children and his passion for long mountain bike rides had to go on the back-burner. He came across a book called “The Obesity Code” by Dr Fung, and decided to implement IF. After consistent weight loss, he became a believer, as did I.
I love the interview between Dr. Fung and Lucy Danzier in her article “Keto Is Dead. Intermittent Fasting Is the Latest Diet Trend, and It Burns Fat Faster”.
Here is an excerpt from her article which includes an interview with Dr. Fung, leading physician in medically-supervised weight loss with IF.
“Dr. Jason Fung trained conventionally in internal medicine at the University of Toronto and then practiced nephrology—the study of kidney diseases such as diabetes and cancer—while at UCLA. Fung learned first-hand from his patients that obesity creates type-2 diabetes and that diabetes, in turn, leads to kidney failure and then dialysis.”
In the interview with Danizer, Dr. Fung writes "At first, I practiced like every other doctor practiced in treating Type 2 Diabetes. What we were doing was treating patients with medication and insulin and it didn't work. I realized that what we were doing was treating it backward. The causality goes from obesity to diabetes to kidney disease and then dialysis. So we have to treat the obesity -- not the kidney failure -- because if you treat obesity then you can reverse type-2 diabetes. I know this because I tried it. And my patients who did it got better. So that's when I started to look at the hormonal underlying or underpinning reasons -- why are so many people obese. It's not about calories. The body isn't having a response to calories. In fact, 100 calories of soda vs. 100 calories of salmon -- the hormonal response to those are not the same at all. Our bodies respond to hormones. The effect of grilled salmon vs. cola or cookies on your body is completely different.
"Predominantly, we are talking about the insulin response in your body. Insulin tells the body to store fat. When you eat, insulin response goes up, and it tells the body to store excess blood sugar as fat. When you don't eat, like when you sleep, insulin levels fall. So you have to mobilize calories from fat to burn energy to live. If you eat too much sugar or too many carbs, you have to store all those calories as fat. After you do that, there is no energy available -- so you go out and eat more. And again, when insulin goes up again, all the new calories are stored as fat.
"Some foods are more fattening and some foods are less fattening. People who eat more salad don't get fat while people who eat more cookies and cake (or any sweets) do get fat. So, the next step is to understand how the hormonal response to the type of food you eat tells your body to store fat or not store fat. This is why people care about the glycemic index (GI) of food. The lower the GI, the less your insulin response spikes.
"If you never let your insulin drop then you never tell your body to pull calories from fat. So there is a whole movement among athletes to training in the fasting state. If you train without eating, then you need to pull calories out of storage to get through an intense workout. If you eat in the morning -- let's say you have a muffin before your workout -- then you use up that source and your body never uses calories from fat and your workout was not effective if the reason you're working out is to lose fat.

"So I started to understand more about insulin. At that point, when I started my studies on Type 2 Diabetes patients, there hadn't been a lot of people talking about it and I started thinking about fasting. If you want to drive your insulin low then that's going to involve fasting. And I thought 'That sounds like a bad idea.' But then I realized that there is a misconception that your body slows down. That does happen on a low-calorie diet, but not when fasting. You're switching your body over to a new fuel system.
"People who cut their calories and go on a low-fat diet are losing all the dietary fat. If you do that and lower your calories to 1,500 -- you may be lowering your intake but since fat has no effect on insulin, if you have 1,500 calories of bread or pasta, the carbs still stimulate an insulin response. But, if you eat whole foods that have fat, such as avocado, it won't stimulate insulin.

"If you fast, and don't eat at all, for 12 or 14 or 16 hours, then your insulin is going to fall-- therefore, your body is going to switch over and naturally burn fat. So your body wants 2,000 calories a day, and your body has maybe 200,000 calories stored (as fat). So your metabolic rate doesn't fall, even without exercise. You just start to burn all those stored calories from fat.
"When we asked patients with Type 2 Diabetes to participate in fasting 24 hours, three times a week, they lost weight and got better. They even got off their meds. And it happened so fast.
"Typically people eat breakfast at 8 am and dinner at 6 pm and in that case, we are already fasting 14 hours a day without thinking about it. In the 70s they ate supper earlier. Even if you eat breakfast at 7 am and dinner at 7 pm then you're fasting at least 12 hours a day. This acknowledges that you're supposed to eat in a cycle. There is a certain number of hours in a day when you are supposed to be eating and a certain number of hours when you are supposed to be fasting.
"If you throw your body out of balance and eat from the minute you get up until the minute you get in bed, then you're only fasting for 8 hours

"If you drink alcohol it is metabolized like sugar, so you have to count wine or beer or spirits in this equation -- so people who drink a lot of wine, they need to know that it's metabolized in the body just like sugar. Two glasses of wine are like having dessert. If you want to lose weight, skip the carbs and the alcohol. Insulin gets mobilized the same way, whether it's carbs in food or the sugar in alcohol. People talk about drinking with dinner -- which is reasonable, except if you're trying to lose weight.
So how does one start intermittent fasting?
I like how Danizer explains fasting options in her aforementioned article.
“Here's the great news,” writes Danizer, “whether you fast for 12, 14 or 16 hours or longer it is completely flexible --- you could push it up to 16 hours, and do it a couple of times a week. So you eat in an 8-hour window, from 11 am to 7 pm and then have 16 hours of fasting. "You can push it up to 24 hours of fasting -- you could have dinner and then fast from 8 p.m. until 8 p.m the next night. That's the one-meal-a-day diet. You still are eating that one meal in a day. Eating is not just for sustenance. It's also for interacting with your family and gives you that time to sit down with your family and be social.”
And if you are up for a longer fast, such as a 3-7 day fast for an extra weight loss push, we can walk you through what that would like in order to keep your electrolyte levels safe. I don NOT advise extended fasting without medical supervision (ie getting baseline and intermittent EKG, labs, blood pressure and heart rate checks--we CAN do all this at Hearthside Medicine).
My husband’s longest fast was 10 days long. This is not IF—this is called an “extended fast.” During this period, we ran a baseline EKG , a half-way point EKG, checked his blood pressure and heart rate and checked what we call a comprehensive metabolic panel—to ensure his sodium and potassium levels were normal and blood sugar not too low. During this fast, he exercised most days, including a 30 mile mountain bike ride one day. Exercise + fasting =biggest weight loss.

We monitored his blood pressure and fasting blood sugar levels and ketones daily. For 10 days, he fasted on lemon water with Himalayan salts, some black coffee, and homemade bone broth. He lost 10 lbs and now, a month later, has kept it off. EKG and blood work is not necessary for IF, when one is eating one meal a day or in a small window), but it is a good idea for extended fasts.
Is fasting safe for everyone?
Intermittent fasting is generally quite safe, but diabetics on insulin should only fast under the very careful scrutiny of their PCP or endocrinologist. I always advise people ask their provider about their plans before starting fasting—some providers are well-versed in IF and others may not know much at all about it.
Fasting can be a game-changer for many conditions and reverse or drastically improve conditions such as diabetes, high cholesterol, high blood pressure, inflammatory bowel issues, and some joint disorders. It has been used as a public health modality in many other countries for decades to treat various medical conditions.
“Oh, I could never fast. I’d get hungry and hangry and bitchy and get low blood sugar. It wouldn’t be pretty.”—I hear this a lot.
“If you don't eat,” reports Danizer, “your hunger subsides in a little while. When your hunger drops, whether you eat or not, it's because your body fed itself from its own fat. Your body gets more efficient at pulling calories from fat. So as you fast your hunger decreases over time. People say, "I got used to it." I think my stomach shrank. But your stomach didn't actually shrink. The body just got better at pulling calories from fat. Your body is learning to fuel itself on its own body fat.It's now fueling itself so efficiently that you won't have the same level of hunger after the first few times you try it."

Danzier goes on to write:
"I tell people to cut out snacking [after dinner], so you get to 14 hours. Then you push it to 16 hours. Typically it's a lot easier to drop breakfast than dinner. If you look at circadian rhythms, hunger is usually at the lowest point at 8 am and it's easy to not eat. At that moment you've gone 12 to 14 hours without eating and you're the least hungry. Your body is fueling itself without food.
"It works well on a plant-based diet. It's only when you add processed or high-carb foods that you have to watch out. You have to be careful about the types of foods you eat since processed foods like wheat and flour, bread is now so processed. For bread now they take the wheat berry and grind it into a fine dust. So the absorption is super quick, unnaturally quick. So if you eat a lot of cakes and cookies and processed breads and donuts,that will spike your insulin. If you're eating a plant-based diet, make sure to keep it whole-food, plant-based, not processed food.

"So if you're plant-based and eating beans, legumes, vegetables and whole grains like quinoa, that all keeps insulin low. If you look at the simple sugars in cereal like Captain Crunch and chocolate donuts that may be vegan but they're terrible for you.
Try Intermittent Fasting for 16 hours. Between 16 and 24 hours twice a week is probably the most popular amount of time.
Our body carries body fat -- so we can use it, says Danizer—“Therefore, if you don't eat you're going to lose it. If you eat all the time you will never lose it. If you watch fit, slim, healthy people, they often cycle through their eating habits. They usually eat with abandon one day and then fast the next.”

I also appreciate the Harvard Health Blog “Intermittent fasting: Surprising update” by Monique Tello, MD, MPH.
She writes, “The food we eat is broken down by enzymes in our gut and eventually ends up as molecules in our bloodstream. Carbohydrates, particularly sugars and refined grains (think white flours and rice), are quickly broken down into sugar, which our cells use for energy. If our cells don’t use it all, we store it in our fat cells as, well, fat. But sugar can only enter our cells with insulin, a hormone made in the pancreas. Insulin brings sugar into the fat cells and keeps it there.
Between meals, as long as we don’t snack, our insulin levels will go down and our fat cells can then release their stored sugar, to be used as energy. We lose weight if we let our insulin levels go down. The entire idea of IF is to allow the insulin levels to go down far enough and for long enough that we burn off our fat.
We have evolved to be in sync with the day/night cycle, i.e., a circadian rhythm. Our metabolism has adapted to daytime food, nighttime sleep. Nighttime eating is well associated with a higher risk of obesity, as well as diabetes.
But why does simply changing the timing of our meals to allow for fasting make a difference in our body? Fasting is evolutionarily embedded within our physiology, triggering several essential cellular functions. Flipping the switch from a fed to fasting state does more than help us burn calories and lose weight…..simple fasting improves metabolism, lowering blood sugar; lessens inflammation, which improves a range of health issues from arthritic pain to asthma; and even helps clear out toxins and damaged cells, which lowers risk for cancer and enhances brain function.”
So what DO I drink while fasting?
I highly advise getting the book "The Obesity Code" by Dr Fung which has this all laid out, but basically, black coffee with just a touch of cream (no artificial stuff or sweetened cream), plain teas, bone broth, and water with unsweetened electrolytes are what you have during your fasting hours. In your non-fasting hours, meals should be simple, lower in carbs (and those carbs should be complex carbs, mostly veggies), lean proteins or plant proteins and healthy fats like avocado, olives, flax seed and flax oil, fish.


Patient Cases
Case one:
“The Philosopher” as we will call him, was a patient of mine who came to me with frustration and distrust. He thought I was going to “lecture him on getting on insulin” because his diabetes was out of control. But he didn’t want to go on insulin, he insisted. “Well, you’re in the right place then,” I told him. “Because I don’t want to put you on insulin except as a last resort. And I’d like to get you off your diabetes medications in general.” He looked at me with skepticism. “If we can get your weight down and change how and when you eat, we can lower your cholesterol AND your blood sugar and likely get you OFF your diabetes medications and keep you from having to go on a statin for high cholesterol. But you have to be willing to work with me diligently on this.
He agreed, and together we met weekly for a couple months while I walked him through the intermittent fasting journey and fine-tuned what he ate.
Within 3 months of IF and exercise, he lost 20 lbs and dropped his blood sugars from a diabetic level to a non-diabetic level. His cholesterol went from a dangerous level needing a statin to a normal level.
Case two:
“The trail runner” –Terry is a hard-core runner who is as fit as fit can be. You wouldn’t know it by looking at him that his blood sugar levels were pre-diabetic and his cholesterol dangerously high. He had a penchant for eating a lot of snacks at work. His twin brother, also an insanely fit athlete, had a severe heart problem while competing in an Iron Man race. Terry came to me because he wanted to “get healthier and avoid heart disease and diabetes.” We started on the IF journey together and cut out his snacking—we replaced his processed foods with whole foods and complex carbs, and within 3 months, we got his “bad cholesterol” (LDLs) from 197 to 140, dropped his triglycerides by 100 points, and increased his “good cholesterol” (HDL) by 10 points.

Case three:
“The Truck Driver” was living on energy drinks and gas station foods. He was obese, diabetic, and had very high cholesterol and blood pressure. He had recently been started on blood pressure medications and diabetes medications. He decided to stop these medications and get serious about his bad habits and lifestyle. He started doing low-carb IF and exercising, and within 3 months, his A1C (a measure of average blood sugar) went from 11.6 to 6.8. A patient is considered diabetic if their A1C is higher than 6.5. His triglycerides (unhealthy fats that greatly increase risk of stroke/heart attac) went from 800 to 200, and his blood pressure and weight normalized.
Interested in trying IF or starting a “work up” for weight loss?
We are accepting new patients and happy to be part of your journey in health!
Havilah Brodhead is a board-certified nurse practitioner who loves being part of a patient's healing journey and offering a judgement-free, holistic approach to whole body care. She is the owner of Hearthside Medicine Family Care, mom of 2, and loves to bike, swim, ski and yoga it up in Bend, Oregon. She is currently accepting new patients and takes most insurances for full family care, children and adults.
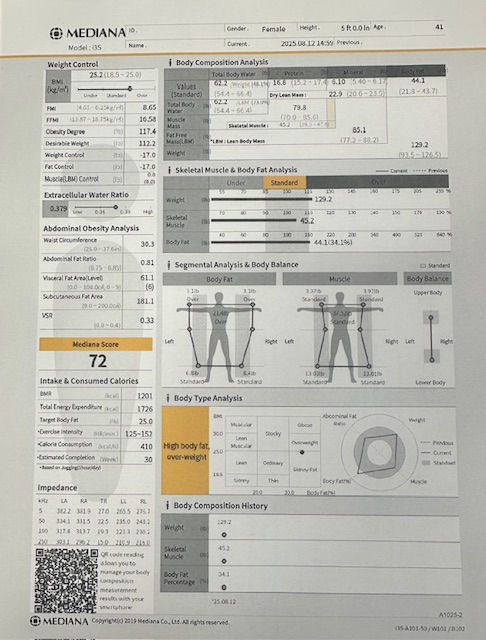




This is the exact program I followed to lower my cholesterol naturally once and for all
( https://lower-cholesterolremedy.weebly.com ). You'll be absolutely thrilled with the step-by-step plan that guides you through the ultimate solution to lower your cholesterol, that you'll only have one regret -- and that is this: Not having had this valuable resource years ago!